That rhythmic thumping or whooshing sound in your ear — the one that pulses in time with your heartbeat — has a name. Doctors call it pulsatile tinnitus, and it affects an estimated 3 to 5 million Americans. Unlike the constant ringing or buzzing of common tinnitus, pulsatile tinnitus beats in rhythm with your pulse. It makes you wonder, “Why can I hear my heartbeat in my ear?” This points to something happening in your blood vessels or surrounding structures, and it nearly always deserves a medical evaluation.
This guide explains why you can hear your heartbeat in your ear, what causes it, when to seek urgent care, and how treatment works. Understanding pulsatile tinnitus is the first step toward getting the right help.

What Is Pulsatile Tinnitus?
Pulsatile tinnitus is a subtype of tinnitus where the sound you hear matches your heartbeat. Most people describe it as a rhythmic whooshing, thumping, or beating sound. It typically occurs in one ear, though both ears can be affected in some conditions.
Standard tinnitus — the persistent ringing or hissing familiar to millions — usually stems from inner ear damage or hearing loss. Pulsatile tinnitus works differently. It originates from actual sound produced by blood flow near the ear, transmitted through bone or tissue into the cochlea. That’s why it pulses: you’re perceiving your own circulation.
To understand the full range of ear-related phantom sounds, our overview of types of tinnitus breaks down how each differs in cause and treatment approach.
What Causes You to Hear Your Heartbeat in Your Ear?
The most common causes of pulsatile tinnitus are vascular. These include carotid artery disease, high blood pressure, idiopathic intracranial hypertension, sinus stenosis, aneurysms, and arteriovenous malformations. Here’s what each means in plain language — and what else can trigger the symptom.
High Blood Pressure
Uncontrolled hypertension is one of the most frequent causes of intermittent pulsatile tinnitus. When blood pressure stays elevated, blood moves through vessels with greater force. That turbulence creates sound the inner ear picks up. Managing blood pressure often reduces or eliminates the symptom. Read more about the connection between hypertension and tinnitus and how vascular health shapes what you hear.
Carotid Artery Disease
Plaque buildup narrows the carotid artery, disrupts smooth blood flow, and generates turbulence close enough to the ear to become audible. Carotid artery stenosis ranks among the most common arterial causes of pulsatile tinnitus, particularly in older adults. The sound typically occurs on the same side as the affected artery.
Idiopathic Intracranial Hypertension
Idiopathic intracranial hypertension (IIH) is elevated pressure in the fluid surrounding the brain without a tumor or other obvious structural cause. When that pressure builds, fluid movement near the ear becomes audible. IIH most commonly affects younger women and often comes with headaches and vision changes alongside the pulsing ear sound.
Arteriovenous Malformations and Fistulas
Abnormal connections between arteries and veins disrupt normal flow patterns. Blood moves through these connections at higher speed and pressure, creating audible turbulence near the cochlea. These are less common causes but carry stroke risk in some cases, making proper diagnosis essential.
Vascular Tumors
Paragangliomas, also called glomus tumors, grow near the jugular foramen or middle ear. They press on nearby blood vessels and create a pulsing sound that sometimes an examiner can hear directly. These tumors are typically benign but require evaluation and ongoing monitoring.
Anemia and Thyroid Conditions
Low red blood cell counts and an overactive thyroid both increase cardiac output. The heart works harder, pumps more forcefully, and the resulting blood flow creates sound near the inner ear. These are among the more treatable causes — addressing the underlying condition often resolves the tinnitus.
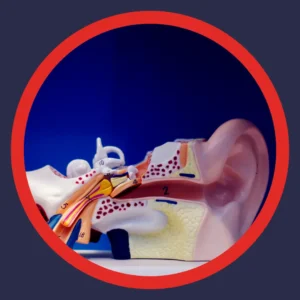
Eustachian Tube Dysfunction and Middle Ear Conditions
Fluid in the middle ear, ear infections, or a patulous Eustachian tube can amplify the sound of blood flow the ear normally filters out. When the tube stays open instead of closing properly, your own heartbeat and breathing can become audible.
Benign Causes
Not every case signals danger. Some people develop temporary pulsatile tinnitus after intense exercise, during pregnancy due to increased blood volume, or during periods of significant stress. In these situations, the sound often resolves once the trigger passes.
What Triggers Pulsatile Tinnitus?
Several factors can bring on or worsen the symptom. The most common triggers include:
- Uncontrolled high blood pressure
- Anemia or significant blood loss
- Intense physical exertion
- Pregnancy and related cardiovascular changes
- Stress and elevated heart rate
- Certain medications that affect blood pressure or flow
- Sleeping positions that compress neck vessels
- Caffeine and stimulant intake in sensitive individuals
Identifying your personal triggers helps a hearing care provider or physician narrow down the underlying cause more efficiently.
Is Pulsatile Tinnitus Serious? When to Act Fast
Most cases of pulsatile tinnitus are not life-threatening, but the symptom always warrants evaluation. Medical literature classifies new-onset pulsatile tinnitus as a red flag because treatable conditions appear in the majority of cases when properly investigated.
Some situations call for urgent or emergency care. Go to the ER or call emergency services if you experience pulsatile tinnitus alongside any of the following:
- Sudden severe headache unlike any you’ve had before
- Vision changes, double vision, or sudden vision loss
- Weakness, numbness, or paralysis on one side of your body
- Difficulty speaking or understanding speech
- Loss of balance or sudden dizziness
- Sudden hearing loss in one ear
These combinations can indicate stroke, aneurysm, or other serious vascular events. Pulsatile tinnitus alone does not mean you’re having a stroke — but paired with neurological symptoms, it demands emergency evaluation.
When to See a Doctor Soon
Schedule a prompt appointment with your primary care provider or an ENT if you notice:
- New pulsatile tinnitus that persists beyond a few days
- One-sided pulsatile tinnitus with no obvious cause
- Pulsatile tinnitus that worsens over time
- Associated hearing changes in the affected ear
- Significant impact on sleep or daily function
What Kind of Doctor Evaluates Pulsatile Tinnitus?
Start with your primary care provider for a blood pressure check and initial workup. Most cases then move to an ear, nose, and throat specialist, who can conduct a hearing evaluation and examine the ear directly. Depending on findings, your care team may expand to include a neurologist, a vascular surgeon, or a neurointerventional specialist.
A hearing care provider also plays an important role in the process. A thorough hearing evaluation helps rule out hearing loss, identify the character of the sound, and guide next steps. Learn more about finding a hearing center near you and what a comprehensive evaluation involves.

How Is Pulsatile Tinnitus Diagnosed?
Diagnosis combines a detailed medical history, physical exam, hearing testing, and imaging. The type of imaging depends on your symptoms and physical findings. Options include:
| Diagnostic Tool | What It Evaluates |
|---|---|
| Audiological evaluation | Hearing thresholds, speech discrimination, sound character |
| Blood pressure measurement | Hypertension as a contributing cause |
| MRI and MR angiography | Brain and blood vessel structure and flow |
| CT with contrast | Bone structures and vascular anatomy near the ear |
| Carotid ultrasound | Stenosis or plaque in the carotid arteries |
| Blood panel | Anemia, thyroid function, and metabolic causes |
No single test rules out all possibilities. A systematic approach matters because causes range from completely benign to medically serious. Recent research on pulsatile tinnitus confirms that a comprehensive clinical and imaging protocol is essential for accurate diagnosis.
Can Pulsatile Tinnitus Go Away?
Yes — pulsatile tinnitus can resolve, and the likelihood depends heavily on the underlying cause. Cases tied to high blood pressure, anemia, thyroid dysfunction, or middle ear fluid often improve significantly when those conditions receive proper treatment. Pregnancy-related pulsatile tinnitus typically fades after delivery as blood volume normalizes.
Cases tied to structural vascular abnormalities may require procedural intervention. Endovascular treatments including stenting, coiling, and embolization have shown strong outcomes in carefully selected patients. Some cases with no identifiable structural cause may persist but stay manageable with sound therapy, lifestyle changes, and stress reduction.
How Hearing Aids Help With Pulsatile Tinnitus
When pulsatile tinnitus coexists with hearing loss — which is common, especially among older adults and veterans — hearing aids play a meaningful role in management. Amplifying environmental sound reduces the relative prominence of the internal pulsing. Many modern hearing aids also include dedicated sound therapy programs that introduce background tones to mask tinnitus perception.
Pulsatile tinnitus appears at higher rates among people with noise-related hearing histories. Veterans face elevated risk from both noise exposure and related vascular changes — read more about veterans and hearing loss and how service history shapes long-term auditory health.
For older adults navigating pulsatile tinnitus alongside age-related hearing loss, explore our guide to hearing aids designed to address tinnitus and which features matter most.
What You Can Do Right Now
You don’t have to wait for symptoms to worsen before taking action. Start here:
- Track your symptoms: note which ear, how often, what triggers it, and whether position changes affect the sound
- Check your blood pressure at a pharmacy or clinic
- Reduce caffeine, stress, and known cardiovascular risk factors
- Avoid sleeping on the affected side if that worsens the sound
- Schedule a hearing evaluation and a medical appointment promptly
Early evaluation leads to clearer answers and better outcomes. At American Hearing + Audiology, our hearing care providers take tinnitus seriously. We carry five premium brands — Phonak, ReSound, Starkey, Oticon, and Unitron — and fit every patient using real ear measurement to verify performance. Our 7-day free trial lets you experience hearing aids before committing. And, we work with most major insurance plans and help you verify your benefits from the start.
In your network. In your neighborhood. In your corner. Find a clinic near you and take the first step today.
FAQs About Hearing Your Heartbeat in Your Ear
How can I stop the heartbeat sound in my ear?
Treatment depends on the cause. Controlling blood pressure often reduces the symptom significantly. Treating anemia, thyroid conditions, or middle ear fluid addresses those specific triggers. Structural causes like carotid stenosis or vascular malformations may require medical or procedural intervention. There’s no proven self-treatment that reliably stops pulsatile tinnitus — identifying and treating the underlying cause is always the goal.
Is pulsatile tinnitus a red flag?
Yes. Medical literature classifies new-onset pulsatile tinnitus as a red flag symptom requiring evaluation. An identifiable and treatable underlying condition exists in the majority of cases. That doesn’t mean every case is dangerous — but investigation always matters.
Does hearing your heartbeat in your ear mean high blood pressure?
High blood pressure is one of the most common causes, but not the only one. Anemia, thyroid conditions, vascular abnormalities, and even posture can produce the same sound. A medical evaluation determines the actual cause.
Is pulsatile tinnitus a sign of stroke?
Pulsatile tinnitus alone is not a stroke symptom. However, if it occurs alongside sudden neurological changes — weakness, slurred speech, vision loss, or severe headache — seek emergency care immediately. Certain vascular conditions that cause pulsatile tinnitus carry elevated stroke risk, which is why proper diagnosis matters.
Can pulsatile tinnitus go away on its own?
Sometimes. Temporary causes like exercise, stress, or pregnancy often resolve without treatment. Cases linked to high blood pressure or thyroid conditions improve with proper medical management. Structural causes typically require specific treatment. Without knowing the cause, there’s no reliable way to predict resolution — evaluation is always the right move.
Does pulsatile tinnitus mean aneurysm?
An aneurysm is one possible cause among many, but not the most common. Most pulsatile tinnitus cases stem from more routine vascular or cardiovascular conditions. Imaging studies during a medical evaluation can identify or rule out an aneurysm when clinical suspicion warrants it.
Do I need to go to the ER for pulsatile tinnitus?
Go to the ER if pulsatile tinnitus appears suddenly alongside neurological symptoms: severe headache, vision changes, weakness, speech difficulty, or loss of balance. Pulsatile tinnitus alone — without those accompanying symptoms — typically warrants a prompt appointment rather than emergency care.
What is mistaken for pulsatile tinnitus?
Several conditions mimic pulsatile tinnitus. Middle ear muscle spasms produce rhythmic sounds not tied to the heartbeat. A patulous Eustachian tube makes breathing sounds audible in the ear. Jaw joint problems create clicking or thumping sensations. Distinguishing true pulsatile tinnitus from these requires a thorough ear exam and hearing evaluation.
Where should I press to try to stop pulsatile tinnitus?
Some people find that gentle pressure on the jugular vein on the affected side temporarily reduces venous pulsatile tinnitus. Providers sometimes use this during evaluation to help identify a venous cause. It is not a treatment, and you should not apply significant pressure to your neck on your own. See a provider for proper evaluation and guidance.
What kind of doctor do I see for pulsatile tinnitus?
Start with your primary care provider for a basic workup. Most cases progress to an ENT specialist for hearing evaluation and ear examination. A hearing care provider contributes valuable audiological data that shapes the diagnostic picture. Depending on findings, a neurologist or vascular specialist may join the care team. Find a clinic near you to start with a hearing evaluation and take the first step toward answers.



